The Clinical and Laboratory Profiles of Neonatal Thrombocytopenia in a Tertiary Neonatal Intensive Care Unit in Baghdad, Iraq
DOI:
https://doi.org/10.32007/jfacmedbaghdad3255Keywords:
Bleeding, Neonatal Thrombocytopenia, Neonatal Intensive Care Unit, Platelet transfusion, Perinatal Asphyxia, SepsisAbstract
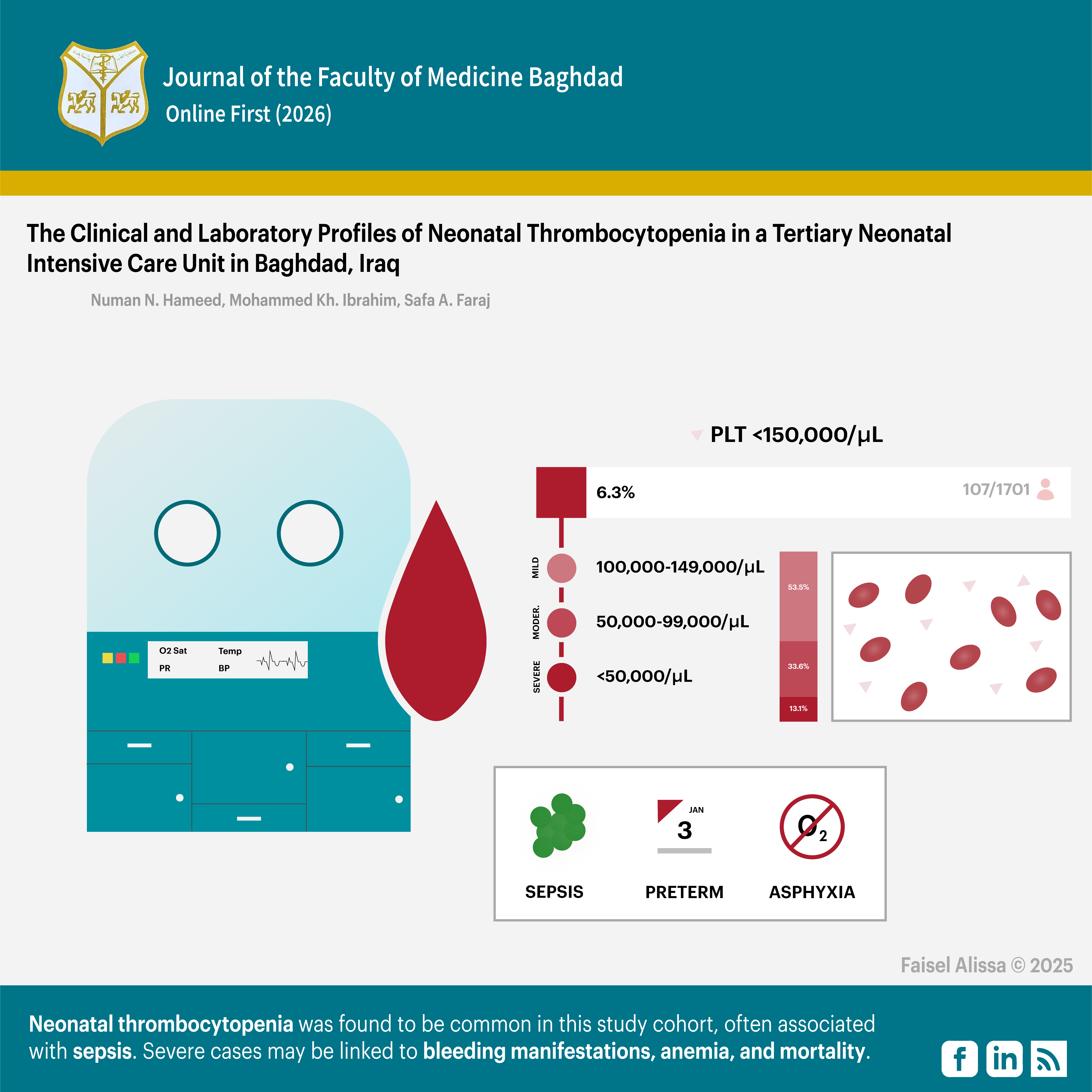
Background: Neonatal Thrombocytopenia (NT) is defined as a platelet count of <150,000/microL and is classified as: Mild (platelet count 100,000- 149,000/microL), moderate (50,000- 99,000/microL), and Severe (<50,000/microL). It is classified according to the time of presentation as: Early NT (occurs within the first 72 hours of life) and Late NT (occurs after 72 hours).
Objectives: To study the clinical and laboratory profiles of neonatal thrombocytopenia in the Neonatal Intensive Care Unit of the Children Welfare Teaching Hospital, Baghdad.
Methods: This single-center case series observational study was conducted from 1st May 2022 to 30th April 2023, in the Neonatal Intensive Care Unit of the Children Welfare Teaching Hospital, Baghdad. Neonates with thrombocytopenia, defined as a platelet count <150,000/µL, were enrolled. Complete blood count, C-reactive protein, blood culture, and other investigations were performed as clinically indicated. Data were analyzed using IBM SPSS version 29. Categorical variables were analyzed using the Pearson chi-square test or Fisher’s exact test, as appropriate, and a P-value of <0.05 was considered statistically significant.
Results: Among the 1701 neonates admitted to the NICU, 107 (6.3%) developed neonatal thrombocytopenia. Mild thrombocytopenia was the most common category, occurring in 57 cases (53.3%), followed by moderate thrombocytopenia in 36 (33.6%) and severe thrombocytopenia in 14 (13.1%). Out of the total cases, there were more preterm 61 (57.0%) than full term neonates 46 (43.0%). Sepsis was the most common associated condition, identified in 53 cases (49.6%), followed by asphyxia in 11 cases (10.3%). Severe thrombocytopenia was significantly associated with hemoglobin <15 g/dL (P=0.04), bleeding from venipuncture and cannula sites (P=0.034), and death (P=0.0001).
Conclusion: Neonatal thrombocytopenia was found to be common in this study cohort, with sepsis being the leading associated condition. Severe cases seem to be linked to bleeding manifestations, anemia, and mortality, which highlight the importance of careful monitoring of affected neonates.
Received: Dec. 2025
Revised: March 2026
Accepted: April 2026
Published Online: April 2026
References
1. Eichenwald EC, Hansen AR, Martin CR, Stark AR. Cloherty and Stark's Manual of Neonatal Care. 9th ed. Philadelphia: Lippincott Williams & Wilkins; 2023.
2. Christensen RD, Baer VL, Henry E, Snow GL, Butler A, Sola-Visner MC. Thrombocytopenia in small-for-gestational-age infants. Pediatrics. 2015;136(2):e361-e370. https://doi.org/10.1542/peds.2014-4182.
3. Christensen RD, Henry E, Wiedmeier SE, Stoddard RA, Sola-Visner MC, Lambert DK, et al. Thrombocytopenia among extremely low birth weight neonates: data from a multihospital healthcare system. J Perinatol. 2006;26(6):348-353. https://doi.org/10.1038/sj.jp.7211509.
4. Baer VL, Lambert DK, Henry E, Christensen RD. Severe thrombocytopenia in the NICU. Pediatrics. 2009;124(6):e1095-e1100. https://doi.org/10.1542/peds.2009-0582.
5. Donato H. Neonatal thrombocytopenia: definitions, differential diagnosis, and causes. Arch Argent Pediatr. 2021;119(3):e202-e214. https://doi.org/10.5546/aap.2021.eng.e202.
6. Morrone K. Thrombocytopenia in the Newborn. Neoreview 2018;19(1):e34–e41. https://doi.org/10.1542/neo.19-1-e34.
7. Stanworth SJ, Mumford AD. How I diagnose and treat neonatal thrombocytopenia. Blood. 2023 Jun 1;141(22):2685-97. https://doi.org/10.1182/blood.2022018017.
8. Won Lee S, Clinton TA, Kim SK. Fetal/neonatal alloimmune-mediated thrombocytopenia and recurrent pregnancy loss. In Immunology of Recurrent Pregnancy Loss and Implantation Failure 2022 Jan 1 (pp. 165-175). Academic Press. https://doi.org/10.1016/B978-0-323-90805-4.00014-6.
9. Sola MC, Del Vecchio A, Rimsza LM. Evaluation and treatment of thrombocytopenia in the NICU. Clin Perinatol. 2000;27(3):655-670. https://doi.org/10.1016/S0095-5108(05)70044-0.
10. Ververidis M, Kiely EM, Spitz L, Drake DP, Eaton, Pierro SA. The clinical significance of thrombocytopenia in neonates with necrotizing enterocolitis. J Pediatr Surg. 2001;36(5):799-803. https://doi.org/10.1053/jpsu.2001.22964.
11. Fressinaud E, Mazurier C, Meyer D. Molecular genetics of type 2 von Willebrand disease. Int J Hematol. 2002;75(1):9-18. https://doi.org/10.1007/BF02981973.
12. Ulusoy E, Tufekci O, Duman N, Kumral A, Irken G, Ören H. Thrombocytopenia in neonates: causes and outcomes. Ann Hematol. 2013;92(7):961-967. https://doi.org/10.1007/s00277-013-1726-0.
13. Kusumasari N, Rohsiswatmo R, Gatot D, Darwis D. Incidence and risk factors of neonatal thrombocytopenia: a preliminary study. Pediatr Int. 2010;50(1):31-37. https://doi.org/10.14238/pi50.1.2010.31-7.
14. Eltawel M, AlHarbi T, AlJamaan K, Alsaif S, Ali Y, Salam M. Incidence and outcomes of neonatal thrombocytopenia in a tertiary care facility. Adv Neonatal Care. 2018;18(5):E3-E12. https://doi.org/10.1097/ANC.0000000000000539.
15. Saber AM, Aziz SP, Almasry AZE, et al. Risk factors for severity of thrombocytopenia in full-term infants. Ital J Pediatr. 2021; 47:7. https://doi.org/10.1186/s13052-021-00965-1.
16. Zekry S, Hamed E, Hassanen F, Abdel-Aziz S. Incidence and risk factors for neonatal thrombocytopenia. Ann Neonatol J. 2022;4(1):7-26. https://doi.org/10.21608/anj.2021.89757.1035.
17. Van der Staaij H, Hooiveld NMA, Caram-Deelder C, Fustolo-Gunnink SF, Fijnvandraat K, Steggerda KS, et al. Most major bleeds in preterm infants occur in the absence of severe thrombocytopenia: an observational cohort study. Arch Dis Child Fetal Neonatal Ed. 2025;110:F122-F127. https://doi.org/10.1136/archdischild-2024-326959.
18. Peng T, Shan Y, Zhang P, Cheng G. Bleeding in neonates with severe thrombocytopenia. BMC Pediatr. 2022; 22:730.
https://doi.org/10.1186/s12887-022-03802-4.
19. Chakravorty S, Roberts I. How I manage neonatal thrombocytopenia. Br J Haematol. 2012;156(2):155-162. https://doi.org/10.1111/j.1365-2141.2011.08892.x.
20. Abate AT, Gedefaw GD, Kassahun CW, Kelkay MM. Prevalence and associated factors of neonatal thrombocytopenia. Sci Rep. 2025; 15:12610. https://doi.org/10.1038/s41598-025-93042-0.
21. Tirupathi K, Swarnkar K, Vagha J. Risk factors of neonatal thrombocytopenia. Int J Contemp Pediatr. 2017;4(1):191-196. https://doi.org/10.18203/2349-3291.ijcp20164603.
22. Mlynarczyk M, Chauhan SP, Baydoun HA, Wilkes CM, Earhart KR, Zhao Y, et al. The clinical significance of an estimated fetal weight below the 10th percentile: a comparison of outcomes of <5th vs 5th-9th percentile. Am J Obstet Gynecol. 2017;217(2):198.e1-198.e11. https://doi.org/10.1016/j.ajog.2017.04.020.
23. Kalagiri RR, Choudhury S, Carder T, Govande V, Beeram MR, Nasir Uddin M. Neonatal thrombocytopenia in maternal preeclampsia. AJP Rep. 2016;6(1):e42-e47. https://doi.org/10.1055/s-0035-1565923.
24. Resch E, Hinkas O, Urlesberger B, Resch B. Neonatal thrombocytopenia outcomes following transfusion. Eur J Pediatr. 2018;177(7):1045-1052. https://doi.org/10.1007/s00431-018-3153-7.
25. Farag MM, Goda MH, Nazir HF, Deghedy AA. Determinants of thrombocytopenia in newborns. BMC Pediatr. 2024;24:805. https://doi.org/10.1186/s12887-024-05170-7.
26. Ankitha C, Kumar SP, Mahendrappa KB, Krishnegowda M. Etiological profile of neonatal thrombocytopenia. Int J Pharm Clin Res. 2023;15(6):1350-1359. https://doi.org/10.5281/zenodo.12510297
27. Jain S, Gaur BK, Sharma M, Singh RR. Thrombocytopenia outcomes in preterm neonates. Iraqi J Hematol. 2024;13:110-117. https://doi.org/10.4103/ijh.ijh_17_24.
28. Patil S, Mangshetty R, Patil B. Outcome of neonates with thrombocytopenia. J Evol Med Dent Sci. 2014;3(17):4533-4538. https://doi.org/10.14260/jemds/2014/2471.
29. Saxonhouse MA, Sola-Visner MC. Thrombocytopenia in NICU. NeoReviews. 2009;10(9):e435. https://doi.org/10.1542/neo.10-9-e435.
30. Ribeiro HS, Assuncao A, Vieira RJ, Soares P, Guimarães H, Flôr-de-Lima F. Platelet transfusions in preterm infants. Eur J Pediatr. 2023; 182:3433-3443. https://doi.org/10.1007/s00431-023-05031-y.
31. Boix H, Sanchez-Redondo MD, Cernada M, Fernández MGE, González-Pacheco N, Martín A, et al. Blood product transfusion in neonatology. An Pediatr (Barc). 2022;97:e1-e8. https://doi.org/10.1016/j.anpede.2022.05.003.
32. Cetinkaya M, Atasay B. Transfusions in neonatal period. Front Pediatr. 2022; 10:982918. https://doi.org/10.3389/fped.2022.982918.
33. Chotas W, Wallman-Stokes A, Patel RM, Cooper C, Soll R. Platelet transfusion thresholds in neonates. Cochrane Database Syst Rev. 2024;(1):CD015341. https://doi.org/10.1002/14651858.CD01534.
34. Davenport PE, Wood TR, Heagerty PJ, Sola-Visner MC, Juul SE, Patel RM. Platelet transfusion and neurodevelopmental outcomes. JAMA Netw Open. 2024;7(1):e2352394. https://doi.org/10.1001/jamanetworkopen.2023.52394.
35. Moore CM, D'Amore A, Fustolo-Gunnink S, Hudson C, Newton A, Santamaria BL, et al. Two- year outcomes following a randomized platelet transfusion trial in preterm infants. Arch Dis Child Fetal Neonatal Ed. 2023;108:F452-F457. https://doi.org/10.1136/archdischild-2022-324915.
36. Curley A, Stanworth SJ, Willoughby K, Fustolo-Gunnink SK, Venkatesh V, Hudson C, et al. Platelet-transfusion thresholds in neonates. N Engl J Med. 2019; 380:242-251. https://doi.org/10.1056/NEJMoa1807320.
37. Metcalf RA, Nahirniak S, Guyatt G, Bathla A, White SK, Al-Riyami AZ, et al. Platelet transfusion guidelines. JAMA. 2025;334(7):606-617. https://doi.org/10.1001/jama.2025.7529.
38. Cortesi V, Lopriore E, Fustolo-Gunnink S. Platelet transfusion and bleeding risk. Semin Fetal Neonatal Med. 2025; 30:101608. https://doi.org/10.1016/j.siny.2025.101608.











 Creative Commons Attribution 4.0 International license..
Creative Commons Attribution 4.0 International license..


